Making Artificial Intelligence (AI) Bullet Proof
SUMMARY:
AI’s prevalence within healthcare has the potential to transform patient care and outcomes.
Due to the persistence of common challenges, deployment of AI in clinical practice remains limited.
Solutions in the development, implementation and post-implementation can help to make AI solutions more trustworthy.
REVIEW
AI Objectives and Use Cases
OBJECTIVES
Improved diagnostic effectiveness
Decreased healthcare costs
Improved information sharing
USE CASES
Diagnostic predictions with early symptom analysis.
Virtual health assistants
Targeted therapy recommendations
Drug Discovery
AI Challenges
TOP CHALLENGES FOR AI
Data Quality & Accessibility
Volume of data ≠ quality & availability
Healthcare data is fragmented across various systems contributing to inaccuracies and inconsistencies
May provide inaccurate insights and recommendations adversely affecting performance and reliability.
Implementation Costs
1. Requires significant investment
Technical infrastructure
Regulatory compliance
Staff training
Acceptance of AI in Healthcare
The AI Chasm: discrepancies in clinical efficacy and usefulness between predicted model in development dataset and real world data
Lack of trust in results
Lack of AI Performance Evaluation
There is a need to assess AI performance before widespread implementation across a health system
Most AI studies are retrospective and based on patient medical record data.
Need reliable measurements of accuracy and reliability
This ongoing gap is a major challenge in determining how well the AI solution meets:
clinical goals,
integration with existing workflows and processes
patient outcomes
impact costs
Regulatory Issues
Keeping up with the ever changing regulatory environment across the globe
Bias
AI algorithms may have inherent bias in economic, social, gender and race
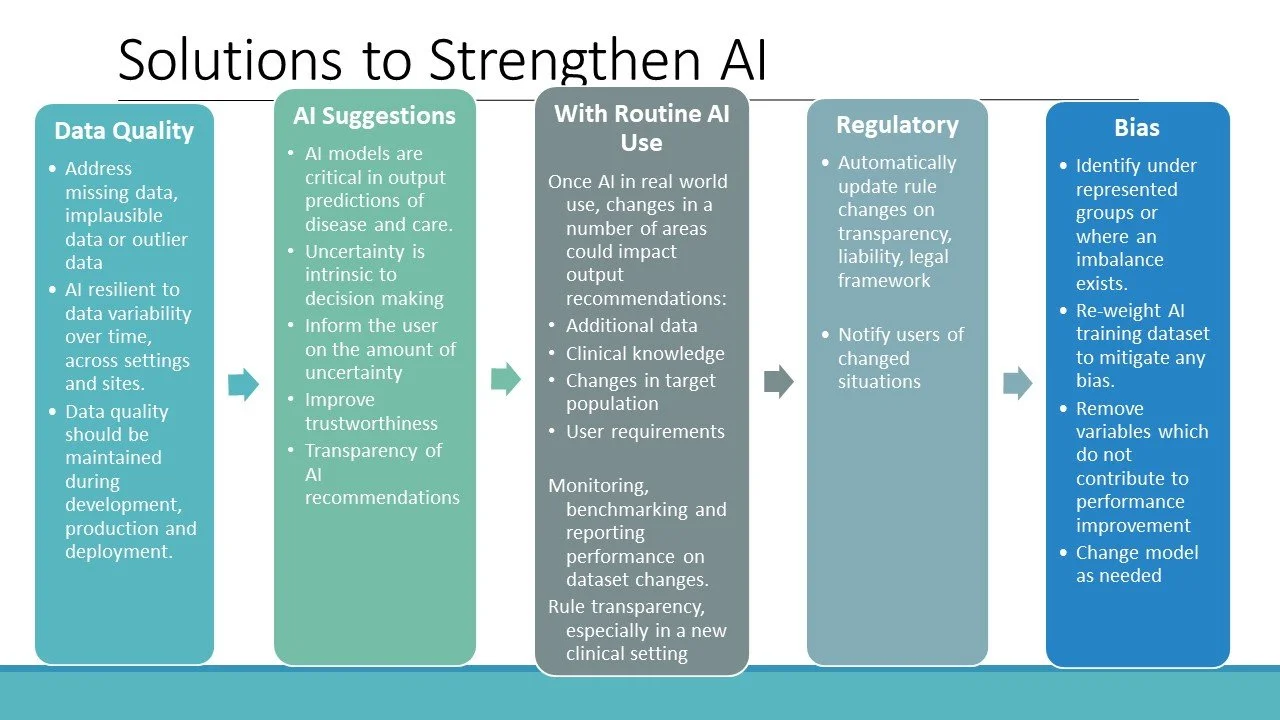
Solutions to Strengthen AI
Data Quality
Missing data; implausible data; outlier data
AI should identify these types of inputs
Allow model to discard or fix
Infer useful information associated with faulty inputs
2. AI should be developed to be resilient to data variability over time, across settings and sites
3. Data quality should be maintained not only during development, but in production as well.
AI Recommendations
Strengthening AI models become critical in output predictions of disease and care.
Uncertainty is intrinsic to decision making.
Minimizing uncertainty or informing the user of the amount of uncertainty improves the trustworthiness of the model
Transparency of why an AI system comes to a final recommendation and provides a specific output from varying inputs improves interpretability.
Ability to compare current clinical scenario to similar past cases and their respective outputs would be helpful
With Routine AI Use
Once AI solution is in real world routine use, changes in a variety of areas may occur impacting output recommendations:
Additional data
Clinical knowledge
Changes in target population
User requirements
2. Monitoring, benchmarking and reporting performance on dataset shifts becomes critical
3. AI systems which can adapt to new knowledge over time, require greater transparency, especially when moved to a new clinical setting
Regulatory
As rules on transparency, liability and legal frameworks evolve, AI systems need to be able to be:
Updated automatically
Notify users of changed situations
How to implement and notify of new rules is left to system designers
Bias
Identify underrepresented sub populations or where an imbalance exists
Re-weight AI training to mitigate the discrimination
Remove variables that do not contribute to output performance
Make changes to model in pre-development; during training of the solution and post-training.
CONCLUSIONS:
There are a number of challenges currently present which preclude the widespread use of AI in clinical care.
Despite these challenges AI will be transformative within health care.
Developing or evaluating AI systems should include the complete assessment of the areas outlined above.