A Specialized Approach to Clinically Evaluate Digital Health Solutions
SUMMARY:
Digital Health Solutions (DHS) play an active role in healthcare delivery.
Most DHS do not have convincing evidence of improved clinical outcomes.
A tailored approach to clinical validation is required due to the complexities associated with DHS use.
REVIEW
DHS can improve health care access, patient equity, operational efficiency and cost effectiveness.
DHS are complex interventions as they are not solely biologic agents (like medications), but rather consist on psychological, behavioral and system level components.
Most DHS lack convincing evidence of impacting clinical outcomes.
Due to their complexities, a specialized approach to their clinical validation is required.
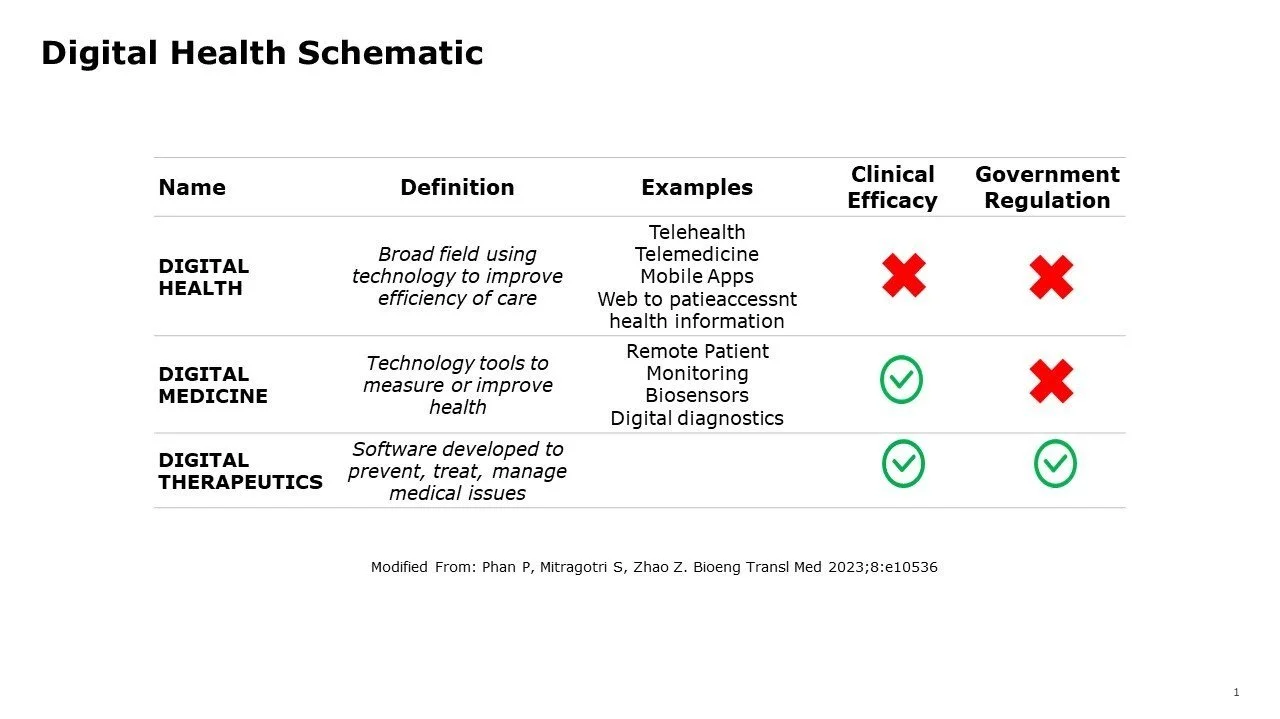
Digital Health Schematic
Unique Characteristics of DHS
Patient and Health Care Provider Involvement
Effective DHS implementation involves patient engagement and health care provider(s).
Providers in a control group may change their behavior over time by learning from the intervention group.
Therefore, it is important to not provide controls at the patient level but at the health care site level as well.
DHS interventions are complex with multiple dependencies.
Health care provider characteristics
Patient-provider relationship
Perceived credibility of the intervention
Delivery modality
Psychological, social, economic and cultural factors
These dependencies are controlled for in randomized controlled trials but not DHS evaluations.
DHS may have multiple clinical outcomes
Increased exercise may have a positive effect on sleep, weight, eating habits, cholesterol, glucose regulation.
The impact of each individual component may be small, but the cumulative benefit may be significant.
Choosing a single clinical endpoint may not capture the full impact of the DHS.
The main DHS feature driving change may vary from patient to patient
Different patients may use different DHS features.
If the DHS is assessed as a whole rather than the specific features, the final assessment may be weakened.
This is especially true for DHS with adaptive algorithms which adjust the intervention over time.
Identification of a clinical impact may require a longer treatment and assessment period.
DHS functionality may change over time with each subsequent release.
Clinical evaluations usually evaluate a fixed version of the DHS, which may limit its external validity.
SUMMARY:
CONCLUSIONS:
DHS lack convincing evidence supporting improved clinical outcomes with use.
The unique characteristics of DHS tools require creative, innovative approaches beyond the typical drug trial format to assess their effectiveness.
Clinicians should be aware of these considerations before implementing DHS solutions into their practice workflows.